Release time :2022-05-26
Source:support@yingchitech.com
Scan:2532
Precise positioning is an important cornerstone for threshold detection and guaranteeing treatment effects of transcranial magnetic stimulation (TMS). At present, there are several commonly used positioning methods, such as the 5cm positioning method and the TMS navigation system. Each positioning method has its own advantages and disadvantages. The 5cm positioning method is convenient and fast but relatively inaccurate while the navigation system is expensive and time-consuming. YINGCHI has designed a positioning cap based on the internationally recognized 10-20 EEG positioning system, which has the advantage of quickly and accurately finding stimulation targets, and is suitable for routine clinical treatment of large samples and brain function exploration.
Positioning Process
1. After the threshold is determined, select the protocol in the YINGCHI TMS software according to the safety screening scale and the patient's condition;
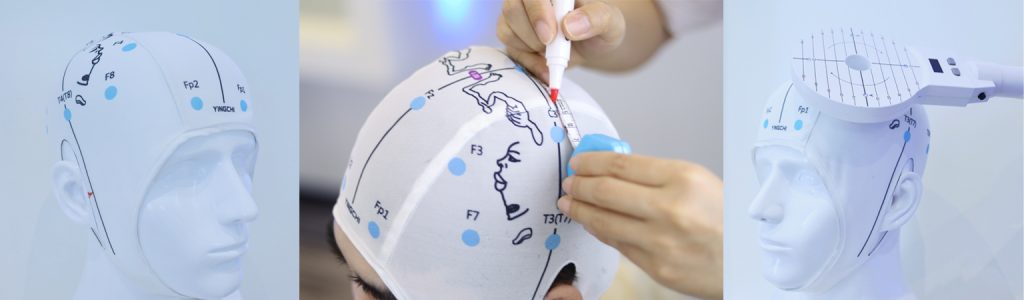
2. Determine the target area and the stimulation site of the positioning cap according to the protocol (see the figure below);
3. Move the coil to make the magnetic field output center coincide with the stimulation target, and the coil must be tangent to the scalp to ensure maximum magnetic field;
4. After adjusting the position, fix the coil and start the treatment according to the parameters of the selected protocol.
Precautions:
1. The operator must ask about patient’s feelings and tolerance to decide whether to adjust the stimulation intensity. If adjustments are required, adjust the intensity in 1% increments during the treatment.
2. Patients must keep their posture unchanged to avoid off-target stimulation in the process.
![TMS stimulation targets and indications based on the international
10-20 system[1]](https://www.yingchi-tms.com/wp-content/uploads/2022/05/图片1-1024x359.png)
| Brain Areas | Left Hemisphere | Right Hemisphere | Brodmann Areas[1,29] | Indications for TMS[30] |
| Orbitofrontal Cortex, OFC | Fp1[2] | Fp2[3] | Area 10 | Depression[31]; OCD[32]; Disturbance of Consciousness After Stroke[33], etc. |
| Dorsolateral Prefrontal Cortex, DLPFC | F3[4] | F4[5] | Area 46 | Depression[34]; Anxious Depression[35]; Parkinson's Disease-Depression[36]; Fibromyalgia[37]; Substance Addiction[38]; Schizophrenia-Negative Symptoms[39]; Disturbance of Consciousness[40]; Insomnia[41]; PTSD[42]; OCD[43], etc. |
| Inferior Frontal Gyrus, IFG | F7[6] | F8[7] | Area 45, 46 | Aphasia After Stroke[44]; ADHD (Language Retardation)[45], etc. |
| Hand Hotspots in Primary Motor Cortex, HH-M1 | C3[8] | C4[9] | Area 4 | Stroke Dyskinesia[46]; Neuropathic Pain[47]; Parkinson’s Disease-Movement Disorder[48]; Disturbance of Consciousness[49]; Fibromyalgia[50]; Dystonia[51]; Multiple Sclerosis[52], etc. |
| Superior Middle Temporal Gyrus, SMTG | T3[10] | T4[11] | Area 21, 22 | Tinnitus[53]; Auditory Hallucination[54], etc. |
| Angular Gyrus of Parietal Occipital Junction, AG-POJ | P3[12] | P4[13] | Area 7 | Hemispatial Neglect After Stroke[55]; Craving for Methamphetamine[56], etc. |
| Superior marginal gyrus, SMG | TP3[14] | TP4[15] | Area 39, 40 | Schizophrenia-Auditory Hallucination[57]; Medication-Resistant Auditory Hallucinations[58]; Psychotic Major Depression-Auditory Hallucination[59] |
| Parahippocampal Gyrus of Posterior Temporal Lobe, PHG-PTL | T5[16] | T6[17] | Area 37, 19, 37, 3 | Alzheimer's Disease-Mild Cognitive Impairment[60]; Tinnitus[61], etc. |
| Supplementary Motor Cortex, SMA | Fz[18] | Fz[18] | Area 6 | Parkinson’s Disease-Movement Disorder[62]; Essential Tremor[63]; Dystonia[64]; Restless Legs Syndrome[65]; Tourette Syndrome[66]; OCD[67], etc. |
| Occipital Lobe | O1[19] | O2[20] | Area 17 | Poststroke Dysphagia[68]; Chronic Stroke-Limbs Dysfunction[69]; Ataxia in Parkinson's Disease[70], etc. |
| Temporoparietal Junction, TPJ | The midpoint of the line T3-P3[21] | The midpoint of the line T4-P4[22] | Area 41, 42 | Chronic Tinnitus[71]; Schizophrenia-Auditory Hallucination[72], etc. |
| Broca's Area | The intersection of the line T3-Fz and the line F7-Cz[23] | The intersection of the line T4-Fz and the line F8-Cz[24] | Area 44, 45 | Aphasia[73]; Post-stroke Aphasia[74]; Alzheimer’s Disease-Cognitive Impairment of Language[75]; Schizophrenia-Auditory Hallucination[76], etc. |
| Wernicke’s Area | The intersection of the line C3-T5 and the line T3-P3[25] | The intersection of the line C4-T6 and the line P4-T4[26] | Area 22 | Alzheimer’s Disease (Language Comprehension Disorder)[75]; Post-stroke Aphasia[77], etc. |
| Swallowing Functional Area of Primary Motor Cortex, SFA-M1 | The midpoint of the line C3-T3[27] | The midpoint of the line C4-T4[28] | Area 4 | Post-stroke Dysphagia[78]; Parkinson’s Disease Dysphagia[79], etc. |
References
1. Homan R W. The 10-20 electrode system and cerebral location[J]. American Journal of EEG Technology, 1988, 28(4): 269-279.
2. Green P E, Loftus A, Anderson R A. Protocol for transcranial direct current stimulation for obsessive-compulsive disorder[J]. Brain Sciences, 2020, 10(12): 1008.
3. Nejati V, Salehinejad M A, Nitsche M A, et al. Transcranial direct current stimulation improves executive dysfunctions in ADHD: implications for inhibitory control, interference control, working memory, and cognitive flexibility[J]. Journal of attention disorders, 2020, 24(13): 1928-1943.
4. Nejati V, Salehinejad M A, Nitsche M A. Interaction of the left dorsolateral prefrontal cortex (l-DLPFC) and right orbitofrontal cortex (OFC) in hot and cold executive functions: Evidence from transcranial direct current stimulation (tDCS)[J]. Neuroscience, 2018, 369: 109-123.
5. Dubreuil-Vall L, Chau P, Ruffini G, et al. tDCS to the left DLPFC modulates cognitive and physiological correlates of executive function in a state-dependent manner[J]. Brain Stimulation, 2019, 12(6): 1456-1463.
6. Hara T, Abo M, Kakita K, et al. The effect of selective transcranial magnetic stimulation with functional near-infrared spectroscopy and intensive speech therapy on individuals with post-stroke aphasia[J]. European Neurology, 2017, 77(3-4): 186-194.
7. Huang Y, Zhang B, Cao J, et al. Potential locations for noninvasive brain stimulation in treating autism spectrum disorders—a functional connectivity study[J]. Frontiers in psychiatry, 2020, 11: 388.
8. Pfurtscheller G, Neuper C, Andrew C, et al. Foot and hand area mu rhythms[J]. International Journal of Psychophysiology, 1997, 26(1-3): 121-135.
9. Hu S, Wang H, Zhang J, et al. Causality from Cz to C3/C4 or between C3 and C4 revealed by Granger causality and new causality during motor imagery[C]//2014 International Joint Conference on Neural Networks (IJCNN). IEEE, 2014: 3178-3185.
10. Steed M, Bigler E D. MRI Brain Atlas[M]//Neuroimaging I. Springer, Boston, MA, 1996: 215-334.
11. Zhang Y, Hauser U, Conty C, et al. Familial risk for depression and p3b component as a possible neurocognitive vulnerability marker[J]. Neuropsychobiology, 2007, 55(1): 14-20.
12. Spitoni G F, Pireddu G, Cimmino R L, et al. Right but not left angular gyrus modulates the metric component of the mental body representation: a tDCS study[J]. Experimental brain research, 2013, 228(1): 63-72.
13. Pick H, Lavidor M. Modulation of automatic and creative features of the Remote Associates Test by angular gyrus stimulation[J]. Neuropsychologia, 2019, 129: 348-356.
14. Xie Y, He Y, Guan M, et al. Impact of low-frequency rTMS on functional connectivity of the dentate nucleus subdomains in schizophrenia patients with auditory verbal hallucination[J]. Journal of Psychiatric Research, 2022, 149: 87-96.
15. Vines B W, Schnider N M, Schlaug G. Testing for causality with transcranial direct current stimulation: pitch memory and the left supramarginal gyrus[J]. Neuroreport, 2006, 17(10): 1047.
16. Sindou M, Guenot M. Surgical anatomy of the temporal lobe for epilepsy surgery[J]. Advances and technical standards in neurosurgery, 2003: 315-343.
17. Velasco A L, Velasco M, Velasco F, et al. Subacute and chronic electrical stimulation of the hippocampus on intractable temporal lobe seizures: preliminary report[J]. Archives of Medical Research, 2000, 31(3): 316-328.
18. Weersink J B, Maurits N M, de Jong B M. EEG time-frequency analysis provides arguments for arm swing support in human gait control[J]. Gait & posture, 2019, 70: 71-78.
19. Sahota P. Occipital Lobes (O1 and O2): Visualizing the World through Recognition and Patterns[M]//Practical Neurocounseling. Routledge, 2020: 171-176.
20. Wang C P, Hsieh P F, Chen C C C, et al. Hyperglycemia with occipital seizures: images and visual evoked potentials[J]. Epilepsia, 2005, 46(7): 1140-1144.
21. Watson N, Jabbour S, Sadler S, et al. Is there an optimal rTMS target to treat chronic tinnitus?[J]. Brain Stimulation: Basic, Translational, and Clinical Research in Neuromodulation, 2021, 14(6): 1689-1690.
22. Mantovani A, Simeon D, Urban N, et al. Temporo-parietal junction stimulation in the treatment of depersonalization disorder[J]. Psychiatry research, 2011, 186(1): 138-140.
23. Monti A, Cogiamanian F, Marceglia S, et al. Improved naming after transcranial direct current stimulation in aphasia[J]. Journal of Neurology, Neurosurgery & Psychiatry, 2008, 79(4): 451-453.
24. Friederici A D, Hahne A, Von Cramon D Y. First-pass versus second-pass parsing processes in a Wernicke's and a Broca's aphasic: electrophysiological evidence for a double dissociation[J]. Brain and language, 1998, 62(3): 311-341.
25. Friederici A D, Hahne A, Von Cramon D Y. First-pass versus second-pass parsing processes in a Wernicke's and a Broca's aphasic: electrophysiological evidence for a double dissociation[J]. Brain and language, 1998, 62(3): 311-341.
26. Marchina S, Schlaug G, Kumar S. Study design for the fostering eating after stroke with transcranial direct current stimulation trial: A randomized controlled intervention for improving dysphagia after acute ischemic stroke[J]. Journal of Stroke and Cerebrovascular Diseases, 2015, 24(3): 511-520.
27. Imperatori C, Fabbricatore M, Innamorati M, et al. Modification of EEG functional connectivity and EEG power spectra in overweight and obese patients with food addiction: An eLORETA study[J]. Brain imaging and behavior, 2015, 9(4): 703-716.
28. Scherer L C, Fonseca R P, Amiri M, et al. Syntactic processing in bilinguals: an fNIRS study[J]. Brain and language, 2012, 121(2): 144-151.
29. Ward J. The student's guide to cognitive neuroscience[M]. psychology press, 2015.
30. Lefaucheur J P, Aleman A, Baeken C, et al. Evidence-based guidelines on the therapeutic use of repetitive transcranial magnetic stimulation (rTMS): an update (2014–2018)[J]. Clinical neurophysiology, 2020, 131(2): 474-528.
31. Schutter D J L G, van Honk J. Increased positive emotional memory after repetitive transcranial magnetic stimulation over the orbitofrontal cortex[J]. Journal of Psychiatry and Neuroscience, 2006, 31(2): 101-104.
32. Ruffini C, Locatelli M, Lucca A, et al. Augmentation effect of repetitive transcranial magnetic stimulation over the orbitofrontal cortex in drug-resistant obsessive-compulsive disorder patients: a controlled investigation[J]. The Primary Care Companion for CNS Disorders, 2009, 11(5): 23968.
33. Bai Y, Xia X, Kang J, et al. Evaluating the effect of repetitive transcranial magnetic stimulation on disorders of consciousness by using TMS-EEG[J]. Frontiers in neuroscience, 2016, 10: 473.
34. Fitzgerald P B, Daskalakis Z J. A practical guide to the use of repetitive transcranial magnetic stimulation in the treatment of depression[J]. Brain Stimulation, 2012, 5(3): 287-296.
35. Du L, Liu H, Du W, et al. Stimulated left DLPFC-nucleus accumbens functional connectivity predicts the anti-depression and anti-anxiety effects of rTMS for depression[J]. Translational psychiatry, 2018, 7(11): 1-10.
36. Randver R. Repetitive transcranial magnetic stimulation of the dorsolateral prefrontal cortex to alleviate depression and cognitive impairment associated with Parkinson's disease: A review and clinical implications[J]. Journal of the Neurological Sciences, 2018, 393: 88-99.
37. Tanwar S, Mattoo B, Kumar U, et al. Repetitive transcranial magnetic stimulation of the prefrontal cortex for fibromyalgia syndrome: a randomised controlled trial with 6-months follow up[J]. Advances in Rheumatology, 2020, 60.
38. Enokibara M, Trevizol A, Shiozawa P, et al. Establishing an effective TMS protocol for craving in substance addiction: Is it possible?[J]. The American journal on addictions, 2016, 25(1): 28-30.
39. Prikryl R, Ustohal L, Kucerova H P, et al. Repetitive transcranial magnetic stimulation reduces cigarette consumption in schizophrenia patients[J]. Progress in Neuro-Psychopharmacology and Biological Psychiatry, 2014, 49: 30-35.
40. Naro A, Russo M, Leo A, et al. A single session of repetitive transcranial magnetic stimulation over the dorsolateral prefrontal cortex in patients with unresponsive wakefulness syndrome: preliminary results[J]. Neurorehabilitation and Neural Repair, 2015, 29(7): 603-613.
41. Jiang C, Zhang T, Yue F, et al. Efficacy of repetitive transcranial magnetic stimulation in the treatment of patients with chronic primary insomnia[J]. Cell biochemistry and biophysics, 2013, 67(1): 169-173.
42. Ahmadizadeh M J, Rezaei M. Unilateral right and bilateral dorsolateral prefrontal cortex transcranial magnetic stimulation in treatment post-traumatic stress disorder: A randomized controlled study[J]. Brain research bulletin, 2018, 140: 334-340.
43. Elbeh K A M, Elserogy Y M B, Khalifa H E, et al. Repetitive transcranial magnetic stimulation in the treatment of obsessive-compulsive disorders: Double blind randomized clinical trial[J]. Psychiatry Research, 2016, 238: 264-269.
44. Hara T, Abo M, Kobayashi K, et al. Effects of low-frequency repetitive transcranial magnetic stimulation combined with intensive speech therapy on cerebral blood flow in post-stroke aphasia[J]. Translational stroke research, 2015, 6(5): 365-374.
45. Qiu A, Li X, Yang Z, Li Z, Wang J, Yuan H, et al. The effects of combined application oftranscranial magnetic stimulation and language training on children withlanguage retardation. Minerva Pediatr. 2016 Oct 28. [Epub ahead of print].
46. Trompetto C, Assini A, Buccolieri A, et al. Motor recovery following stroke: a transcranial magnetic stimulation study[J]. Clinical Neurophysiology, 2000, 111(10): 1860-1867.
47. Knotkova H, Cruciani R A. Non-invasive transcranial direct current stimulation for the study and treatment of neuropathic pain[M]//Analgesia. Humana Press, Totowa, NJ, 2010: 505-515.
48. LEE D H, PARK K W, PARK M K, et al. Transcranial magnetic stimulation in Parkinson's disease[J]. Journal of the Korean Neurological Association, 1999: 352-358.
49. Xie Y, Zhang T. Repetitive transcranial magnetic stimulation improves consciousness disturbance in stroke patients: A quantitative electroencephalography spectral power analysis[J]. Neural Regeneration Research, 2012, 7(31): 2465.
50. Khedr E M, Omran E A H, Ismail N M, et al. Effects of transcranial direct current stimulation on pain, mood and serum endorphin level in the treatment of fibromyalgia: A double blinded, randomized clinical trial[J]. Brain stimulation, 2017, 10(5): 893-901.
51. Siebner H R, Filipovic S R, Rowe J B, et al. Patients with focal arm dystonia have increased sensitivity to slow‐frequency repetitive TMS of the dorsal premotor cortex[J]. Brain, 2003, 126(12): 2710-2725.
52. Mori F, Codecà C, Kusayanagi H, et al. Effects of anodal transcranial direct current stimulation on chronic neuropathic pain in patients with multiple sclerosis[J]. The journal of pain, 2010, 11(5): 436-442.
53. Folmer R L, Carroll J R, Rahim A, et al. Effects of repetitive transcranial magnetic stimulation (rTMS) on chronic tinnitus[J]. Acta Oto-Laryngologica, 2006, 126(sup556): 96-101.
54. Chibbaro G, Daniele M, Alagona G, et al. Repetitive transcranial magnetic stimulation in schizophrenic patients reporting auditory hallucinations[J]. Neuroscience letters, 2005, 383(1-2): 54-57.
55. Kim B R, Chun M H, Kim D Y, et al. Effect of high-and low-frequency repetitive transcranial magnetic stimulation on visuospatial neglect in patients with acute stroke: a double-blind, sham-controlled trial[J]. Archives of physical medicine and rehabilitation, 2013, 94(5): 803-807.
56. Liu Q, Shen Y, Cao X, et al. Either at left or right, both high and low frequency rTMS of dorsolateral prefrontal cortex decreases cue induced craving for methamphetamine[J]. The American journal on addictions, 2017, 26(8): 776-779.
57. JUNG K H, CHOI C S, PARK J S, et al. Effects of repetitive transcranial magnetic stimulation to temporoparietal cortex in patients with chronic schizophrenia with treatment-resistant auditory hallucinations[J]. Journal of Korean Neuropsychiatric Association, 2004: 546-551.
58. Hoffman R E, Hawkins K A, Gueorguieva R, et al. Transcranial magnetic stimulation of left temporoparietal cortex and medication-resistant auditory hallucinations[J]. Archives of general psychiatry, 2003, 60(1): 49-56.
59. Freitas C., Pearlman C., Pascual-Leone, A., 2012. Treatment of auditory verbal hallucinations with transcranial magnetic stimulation in a patient with psychotic major depression: one-year follow-up. Neurocase 18 (1), 57–65.
60. Chang C H, Lane H Y, Lin C H. Brain stimulation in Alzheimer's disease[J]. Frontiers in Psychiatry, 2018, 9: 201.
61. Plewnia C, Bartels M, Gerloff C. Transient suppression of tinnitus by transcranial magnetic stimulation[J]. Annals of Neurology: Official Journal of the American Neurological Association and the Child Neurology Society, 2003, 53(2): 263-266.
62. Boylan L S, Pullman S L, Lisanby S H, et al. Repetitive transcranial magnetic stimulation to SMA worsens complex movements in Parkinson's disease[J]. Clinical Neurophysiology, 2001, 112(2): 259-264.
63. Lu M K, Chiou S M, Ziemann U, et al. Resetting tremor by single and paired transcranial magnetic stimulation in Parkinson’s disease and essential tremor[J]. Clinical Neurophysiology, 2015, 126(12): 2330-2336.
64. Siebner H R, Filipovic S R, Rowe J B, et al. Patients with focal arm dystonia have increased sensitivity to slow‐frequency repetitive TMS of the dorsal premotor cortex[J]. Brain, 2003, 126(12): 2710-2725.
65. Altunrende B, Yildiz S, Cevik A, et al. Repetitive transcranial magnetic stimulation in restless legs syndrome: preliminary results[J]. Neurological Sciences, 2014, 35(7): 1083-1088.
66. Kahl C K, Kirton A, Pringsheim T, et al. Bilateral transcranial magnetic stimulation of the supplementary motor area in children with Tourette syndrome[J]. Developmental Medicine & Child Neurology, 2021, 63(7): 808-815.
67. Mantovani A, Simpson H B, Fallon B A, et al. Randomized sham-controlled trial of repetitive transcranial magnetic stimulation in treatment-resistant obsessive–compulsive disorder[J]. The The International Journal of Neuropsychopharmacology, 2010, 13(2): 217-227.
68. Vasant D H, Sasegbon A, Michou E, et al. Rapid improvement in brain and swallowing behavior induced by cerebellar repetitive transcranial magnetic stimulation in poststroke dysphagia: A single patient case‐controlled study[J]. Neurogastroenterology & Motility, 2019, 31(7): e13609.
69. Liao L Y, Xie Y J, Chen Y, et al. Cerebellar theta-burst stimulation combined with physiotherapy in subacute and chronic stroke patients: a pilot randomized controlled trial[J]. Neurorehabilitation and Neural Repair, 2021, 35(1): 23-32.
70. Carrillo F, Palomar F J, Conde V, et al. Study of cerebello-thalamocortical pathway by transcranial magnetic stimulation in Parkinson's disease[J]. Brain stimulation, 2013, 6(4): 582-589.
71. Schoisswohl S, Langguth B, Hebel T, et al. Personalization of Repetitive Transcranial Magnetic Stimulation for the Treatment of Chronic Subjective Tinnitus[J]. Brain Sciences, 2022, 12(2): 203.
72. Vercammen A, Knegtering H, Liemburg E J, et al. Functional connectivity of the temporo-parietal region in schizophrenia: effects of rTMS treatment of auditory hallucinations[J]. Journal of psychiatric research, 2010, 44(11): 725-731.
73. Naeser M A, Martin P I, Nicholas M, et al. Improved picture naming in chronic aphasia after TMS to part of right Broca’s area: an open-protocol study[J]. Brain and language, 2005, 93(1): 95-105.
74. Szaflarski J P, Vannest J, Wu S W, et al. Excitatory repetitive transcranial magnetic stimulation induces improvements in chronic post-stroke aphasia[J]. Medical science monitor: international medical journal of experimental and clinical research, 2011, 17(3): CR132.
75. Sabbagh M, Sadowsky C, Tousi B, et al. Effects of a combined transcranial magnetic stimulation (TMS) and cognitive training intervention in patients with Alzheimer's disease[J]. Alzheimer's & Dementia, 2019.
76. Kim E J, Yeo S, Hwang I, et al. Bilateral repetitive transcranial magnetic stimulation for auditory hallucinations in patients with schizophrenia: a randomized controlled, cross-over study[J]. Clinical Psychopharmacology and Neuroscience, 2014, 12(3): 222.
77. Versace V, Schwenker K, Langthaler P B, et al. Facilitation of Auditory Comprehension After Theta Burst Stimulation of Wernicke's Area in Stroke Patients: A Pilot Study[J]. Frontiers in Neurology, 2020, 10: 1319.
78. Khedr E M, Abo‐Elfetoh N, Rothwell J C. Treatment of post‐stroke dysphagia with repetitive transcranial magnetic stimulation[J]. Acta Neurologica Scandinavica, 2009, 119(3): 155-161.
79. Khedr E M, Mohamed K O, Soliman R K, et al. The effect of high-frequency repetitive transcranial magnetic stimulation on advancing Parkinson’s disease with dysphagia: double blind randomized clinical trial[J]. Neurorehabilitation and neural repair, 2019, 33(6): 442-452.